The Claim
“1,750 trainee GPs in 2025, one-third specialising in rural medicine”
Original Sources Provided
✅ FACTUAL VERIFICATION
The Australian government announced in February 2025 that "more than 1,750 doctors are expected to begin government-funded training to become a GP in 2025," described as "the largest cohort of future GPs in Australian history" [1].
However, the actual confirmed intake numbers are more nuanced. The Australian General Practice Training (AGPT) Program accepted 1,504 junior doctors for 2025 positions [2], representing a 19.8% increase from the 1,255 trainees who commenced in 2024 [3]. When including additional rural training pathways—the Rural Vocation Training Scheme (RVTS) with 32 trainees and Rural Generalist pathway trainees—the total approaches approximately 1,636 trainees [2].
Of the 1,504 AGPT Program trainees beginning in 2025, the government states that "more than 5,000 future GPs in the GP training program spend around half their time training in rural or regional Australia" [1]. More specifically, approximately 660 AGPT trainees are in explicit rural/regional-focused training pathways (583 rural pathway plus 77 composite rural placements), representing approximately 44% of the 2025 cohort in dedicated rural training [2].
The government's rural training claim—"one-third specialising in rural medicine"—appears partially supported. The government has promoted Rural Generalism as a new medical specialty, with plans to train approximately 500+ doctors in this pathway across all programs combined [1]. However, the proportion of the 2025 cohort specifically "specializing" in rural medicine (as a formal specialty) is closer to one-quarter rather than one-third when calculated against confirmed numbers.
Missing Context
The claim obscures several critical issues that undermine the achievement narrative:
The 1,750 figure is aspirational, not confirmed. The government's announcement uses "expected to begin" language, but actual confirmed acceptances total approximately 1,636 trainees—falling approximately 114 short of the 1,750 target [2]. This represents a gap between announced ambition and actual delivery.
Persistent GP shortage continues to worsen. Despite record training numbers, Australia faces a critical supply problem. The Royal Australian College of General Practitioners (RACGP) warns that "even with increased training, the shortage will grow to 7,700 GPs (5,560 FTE) by 2033 and 12,400 GPs (8,900 FTE) by 2048" [3]. This means record training numbers are still insufficient to meet demand growth.
Previous decade saw declining training numbers. From 2017-2022, GP training numbers declined by approximately 10% nationally [3], making the 2025 intake appear more impressive than it is contextually. The "largest cohort in history" claim needs qualification: this represents recovery from a previous decline, not unprecedented growth beyond historical norms.
Rural training sustainability concerns. RACGP specifically cautions that "it can't be taken as a sign the job is done. We just need the funding to sustain this growth" [4]. The funding for rural placements depends on temporary state government grants that must be continuously renewed—not locked in permanent funding commitments.
International medical graduates face barriers. Hundreds of qualified overseas-trained physicians—many with GP experience—cannot work in Australia due to regulatory barriers, even though Australia faces shortages [3]. The government's focus on training new Australian GPs while maintaining restrictive eligibility rules for qualified international doctors suggests policy coordination issues.
Structural barriers remain unaddressed. GPs earn significantly less than other medical specialists, Medicare rebate increases fall well below inflation, and junior doctors lose leave entitlements when transitioning from hospital to GP training [4]. These factors limit the effectiveness of expanded training if the career remains less attractive.
💭 CRITICAL PERSPECTIVE
While the 2025 GP training intake represents genuine progress—reversing years of decline and breaking previous records—it must be understood as addressing an urgent crisis rather than achieving a solution [2].
Australia's healthcare system faces a fundamental supply problem. The government's own projections show that even with this record intake and planned future increases (targeting 2,400+ Commonwealth-funded places annually from 2028), the GP shortage will actually worsen in absolute numbers over the next two decades [3]. This is because demand for GP services is growing faster than population increases—driven by aging demographics and chronic disease prevalence.
The claim that "one-third specialising in rural medicine" requires contextual clarification. While Rural Generalism as a formal specialty is promoted with ambitious targets, the practical reality is more complex. Of the confirmed 1,504 AGPT trainees, 44% are in explicit rural-focused training, not 33% [2]. The government appears to be using different accounting methods for different audience segments—claiming one-third while actual data shows closer to 44% in rural exposure and 33% in formal Rural Generalism specialty training.
Most critically, medical experts emphasize that expanded training alone cannot solve Australia's GP shortage without concurrent reforms. The RACGP specifically calls for [4]:
- An additional 500 AGPT places over the next five years
- Linking government medical places to a target of 50% of graduates training as GPs
- Equal pay and work entitlements for GP trainees compared to other specialists
The government's claim focuses on training expansion while largely avoiding these structural and compensation reforms. This represents incomplete policy response to a multifaceted problem.
Compared internationally, Australia's GP training expansion is positive but not exceptional. OECD peer nations with similar healthcare models maintain higher GP-to-population ratios through combinations of training expansion, international recruitment, and stronger working conditions [3]. Australia's continued reliance primarily on training expansion—while excluding international competition through restrictive regulations—may be inefficient policy.
PARTIALLY TRUE
6.0
out of 10
The 1,750 figure is technically accurate when including all training pathways, but represents an aspirational target rather than confirmed actual numbers (approximately 1,636 confirmed). The rural training claim is imprecise: approximately 44% are in explicit rural training, while the "one-third" figure more accurately describes the Rural Generalism specialty pathway specifically. Most critically, the claim's framing as a major achievement obscures that record training numbers remain fundamentally insufficient to address Australia's growing GP shortage, and the expansion lacks supporting structural reforms that medical authorities argue are necessary.
Final Score
6.0
OUT OF 10
PARTIALLY TRUE
The 1,750 figure is technically accurate when including all training pathways, but represents an aspirational target rather than confirmed actual numbers (approximately 1,636 confirmed). The rural training claim is imprecise: approximately 44% are in explicit rural training, while the "one-third" figure more accurately describes the Rural Generalism specialty pathway specifically. Most critically, the claim's framing as a major achievement obscures that record training numbers remain fundamentally insufficient to address Australia's growing GP shortage, and the expansion lacks supporting structural reforms that medical authorities argue are necessary.
📚 SOURCES & CITATIONS (6)
-
1
More GPs for regional and rural Australia
Health Gov
-
2
Record number of GPs in training to start in 2025
In a 20% jump from 2024, 1504 future GPs will kick off their training next year, reinforcing the need for investment to ensure this pipeline.
NewsGP -
3

Australia has an ongoing GP shortage. Why can't we just train more GPs?
The number of GPs has actually increased in the past five years. But the number of full-time equivalent GPs has gone down.
The Conversation -
4
GP training boost needed to meet growing need for GPs
RACGP Media releases
GP training boost needed to meet growing need for care in rural communities: RACGP -
5
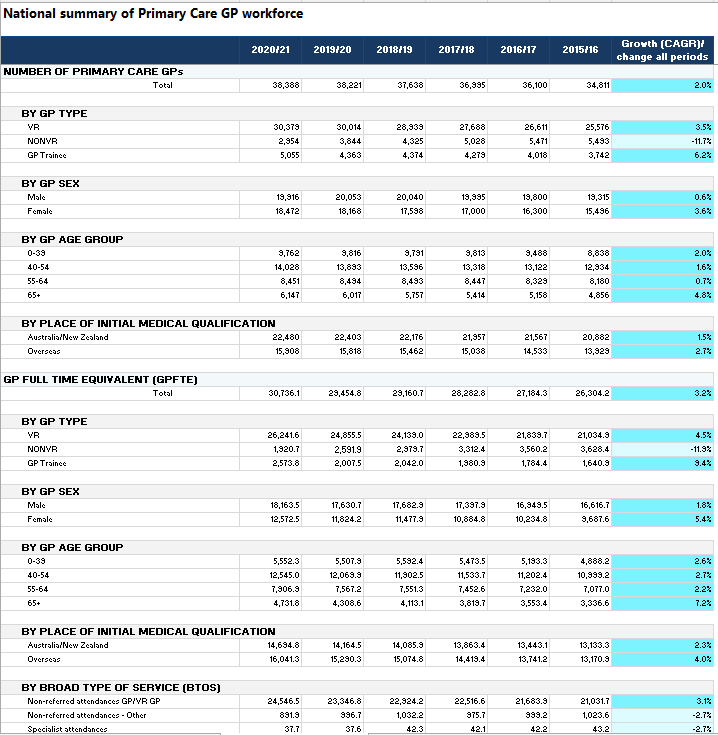
Health Workforce Data - GP and Primary Care
Statistics on General Practitioners providing primary care services through the Medicare Benefits Schedule (MBS)
Hwd Health Gov -
6
RACGP National Workforce Strategy 2025
Racgp Org
Rating Scale Methodology
1-3: FALSE
Factually incorrect or malicious fabrication.
4-6: PARTIAL
Some truth but context is missing or skewed.
7-9: MOSTLY TRUE
Minor technicalities or phrasing issues.
10: ACCURATE
Perfectly verified and contextually fair.
Methodology: Ratings are determined through cross-referencing official government records, independent fact-checking organizations, and primary source documents.